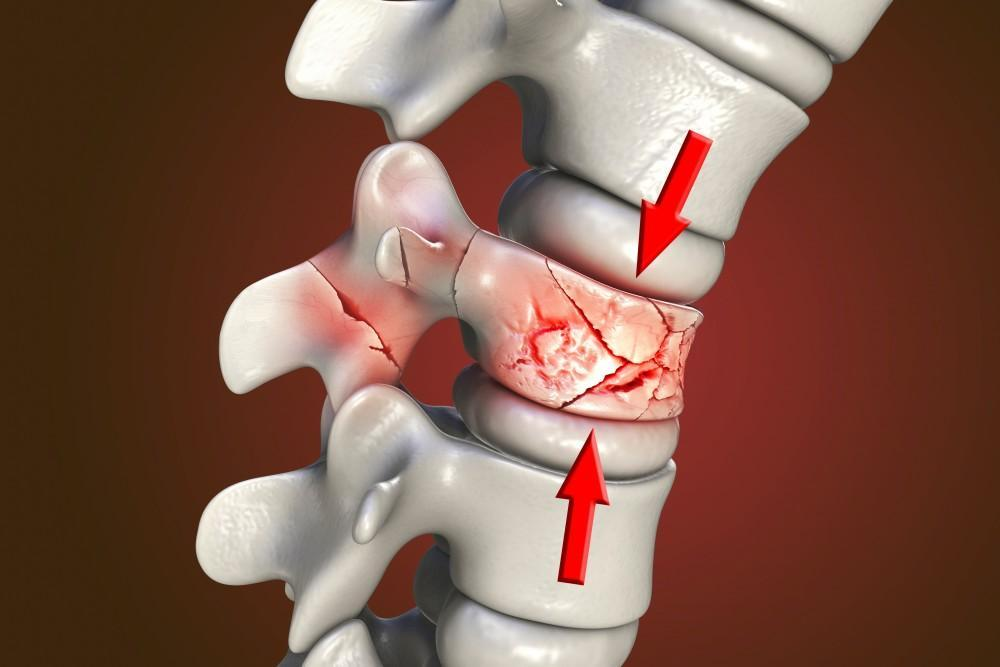
Back pain can change your whole life. It can make it hard to walk, sit, or even sleep. For many people, the pain comes from something called a spinal compression fracture. This is common in people with osteoporosis, especially older adults.
If you or someone you know is dealing with this kind of pain, you may have heard about kyphoplasty. But what is it? And more importantly, is it the right treatment for you?
In this guide, we’ll explain everything in simple terms. We’ll talk about how kyphoplasty works, who it helps, and what you can expect. We’ll also compare it with other options so you can make a smart decision.
What Is Kyphoplasty and When Is It Needed
Understanding Spinal Compression Fractures
A spinal compression fracture happens when one of the bones in your spine, called a vertebra, collapses. This can cause:
- Sudden back pain
- Loss of height
- A hunched posture
The most common cause is osteoporosis, a condition that weakens bones. Even a small fall or simple movement can lead to a fracture.
How Kyphoplasty Helps Relieve Pain Quickly
Kyphoplasty is a minimally invasive procedure. That means it does not need large cuts or long hospital stays.
Here’s how it works:
- A small balloon is placed inside the damaged vertebra
- The balloon is gently inflated to create space
- A special bone cement is injected to stabilize the bone
This helps reduce pain and restore some of the spine’s height. Many patients feel relief within a short time.
Who Should Consider This Procedure
Kyphoplasty is often recommended for people who:
- Have painful vertebral fractures
- Do not improve with rest or medication
- Have pain that limits daily activities
Doctors may also look at your age, bone health, and overall condition before suggesting this treatment.
Conditions Treated with These Procedures
Herniated Discs and Nerve Pressure
While kyphoplasty is mainly used for fractures, other spine issues like herniated discs can also cause back pain. These happen when a disc presses on nearby nerves.
However, kyphoplasty is not usually used for disc problems. It is more focused on bone damage.
Spinal Fractures from Osteoporosis
This is the main condition treated with kyphoplasty. People with osteoporosis often develop weak bones that break easily.
Fixing these fractures can greatly improve comfort and mobility.
Chronic Back Pain That Doesn’t Improve
If your back pain lasts for weeks or months and does not get better with basic care, it may be linked to a hidden fracture.
In such cases, kyphoplasty may offer relief when other treatments fail.
Benefits Compared to Traditional Surgery
Smaller Cuts and Less Pain
Unlike open surgery, kyphoplasty uses tiny tools. This means:
- Less tissue damage
- Smaller scars
- Less pain after the procedure
Faster Recovery and Shorter Hospital Stay
Most people go home the same day or within 24 hours. You can often return to light activities quickly.
This is a big advantage over traditional spine surgery, which may need weeks of recovery.
Better Accuracy and Long-Term Results
With modern imaging tools like fluoroscopy, doctors can guide the procedure with high accuracy.
This improves outcomes and reduces the risk of complications.
What to Expect Before, During, and After Treatment
Preparing for Kyphoplasty
Before the procedure, your doctor may:
- Review your medical history
- Order imaging tests like X-rays or MRI
- Check your bone density
You may also be asked to stop certain medications.
What Happens During the Procedure
During kyphoplasty:
- You will lie on your stomach
- Local or light anesthesia is used
- The doctor inserts a small tube into the spine
- The balloon and cement are placed carefully
The whole process usually takes about one hour per treated vertebra.
Recovery Time and Daily Activity Tips
After the procedure:
- You may feel relief within days
- Light walking is encouraged
- Heavy lifting should be avoided
Most people return to normal routines fairly quickly.
Risks and Safety Considerations
Common Side Effects You Should Know
Like any medical procedure, kyphoplasty has some risks. These may include:
- Mild soreness at the injection site
- Temporary discomfort
- Rare leakage of bone cement
However, serious complications are uncommon.
When to Talk to Your Doctor
You should contact your doctor if you notice:
- Increased pain
- Fever
- Difficulty moving
Early care helps prevent bigger problems.
How to Reduce Risks Before Surgery
To stay safe:
- Follow all medical advice
- Share your full health history
- Choose an experienced specialist
These steps improve your chances of a smooth recovery.
Who Is the Right Candidate for These Treatments
Age, Health, and Medical History Factors
Older adults with osteoporosis are the most common candidates for kyphoplasty.
Your doctor will also check:
- Overall health
- Bone strength
- Severity of the fracture
When Surgery Is the Best Option
If pain is severe and limits daily life, and other treatments do not help, kyphoplasty may be the best choice.
It offers quick relief and helps restore function.
Alternatives You Can Consider First
Before surgery, doctors may suggest:
- Pain medication
- Physical therapy
- Bracing
If these options fail, then kyphoplasty becomes a stronger option.
Conclusion
So, is kyphoplasty the right treatment for spinal compression fractures and chronic back pain?
For many people, the answer is yes. It is a safe, effective, and minimally invasive way to treat painful vertebral fractures, especially those caused by osteoporosis.
It offers quick pain relief, faster recovery, and improved quality of life. But it is not for everyone. The best choice depends on your condition, health, and medical advice.
If you are dealing with ongoing back pain, don’t ignore it. Talk to a healthcare provider and explore your options. The right treatment can help you move better, feel better, and get back to your daily life.